Laparoscopic Gastric Banding
Laparoscopic gastric banding
PATIENT INFORMATION
A gastric band is a life changing operation. It is used to help people to lose weight and improve their health. Losing weight lowers the risk of developing medical problems associated with obesity. For example, high blood pressure, diabetes, arthritis, breathing problems and asthma.
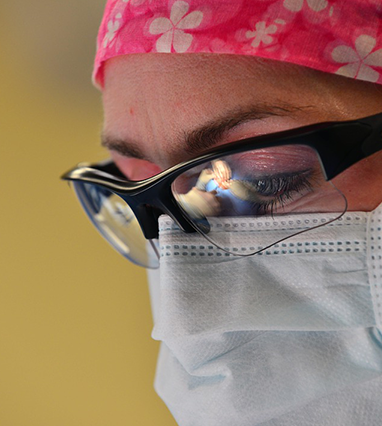
HOW DOES IT WORK?
A gastric band is an inflatable silicone ring which can be used to control the amount of food passing from the stomach into the digestive tract. The operation is done as a laparoscopic (‘keyhole’ surgery) procedure while you sleep under a general anaesthetic. When the ring is placed around the upper part of the stomach, it creates a small pouch at the top of the stomach with a small opening, or ‘channel’, to the rest of the stomach. The size of the pouch and the channel both depend upon how much the ring is inflated.
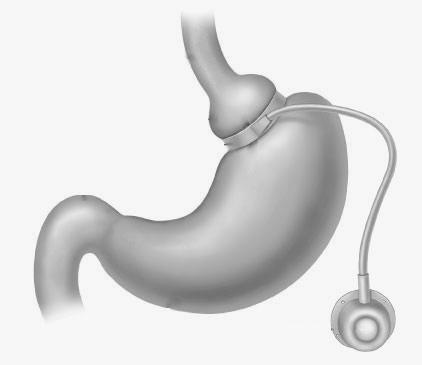
During a meal, food enters the pouch before passing through the opening into the main part of the stomach. The rate at which food passes through depends on the size of the channel between the pouch and the main part of the stomach. The more the ring is inflated, the smaller the opening and therefore the food passes through more slowly.
There is a small port attached by thin tubing to the band. This port is placed just under the skin allowing the band to be adjusted as necessary. Fluid can then be injected or withdrawn to adjust the size of the opening between the upper and lower parts of the stomach. This enables you to feel full sooner and for longer. Vomiting/Band intolerance
1. Feeling full quicker and for longer than usual
2. The procedure is less invasive and easier to reverse than other surgical techniques designed to aid weight loss.
3. The band is adjustable, so we can vary the size of the opening between the pouch and the main part of the stomach if necessary
4. Shorter stay in hospital and shorter recovery time compared to the other procedures
HOW MUCH WEIGHT CAN YOU EXPECT TO LOSE?
You can expect to lose between 40% and 65% of your excess weight in the first 12–24 months following surgery: However a greater excess weight loss is not uncommon in patients who do intensive exercising.
- A man who weighs 146 kg (22 st 13lbs) and is 1.85 m (6’ 1’’) tall has a BMI of 42 kg/m2
- The upper limit of the ideal BMI (25 kg/m2) would give him a weight of 85.6 kg (13 st 6lbs)
- A 50% excess weight loss = 30.2 kg, with a weight of 115.8 kg (18 st 3lbs) (BMI 34 kg/m2)
The amount of weight you are able to lose and keep off after surgery will depend also on the lifestyle changes that you make, such as increasing the amount of exercise you do and eating a healthy diet. It is important to remember that the operation will not stop you from craving certain foods or eating what you fancy.
WHAT ARE THE RISKS OF A GASTRIC BAND?
As with all surgery gastric band has some risks. These risks vary according to your age and other illnesses you may have.
The risk of death within the first 30 days after surgery is estimated to occur in less than 0.05% (or 1 in every 2000 patients) having this operation. This number does not reflect the experience of our surgeons but it is calculated on national and international averages on the base of large multicentre databases. Other short term complications, listed below, happen in less than 5% of patients.
COMPLICATIONS THAT CAN OCCUR SOON AFTER SURGERY
- Wound infection: this can usually be treated with a course of antibiotics and does not require hospital admission.
- Infection of the port or the Band This is usually treated with antibiotics. However, it may be required to remove the port or the band for cleaning the infection.
- Bleeding: Very rare after gastric band. You will be monitored carefully for signs of bleeding. If occurs, it can be often managed conservatively and occasionally it may require transfusions.
- Blood clots in the legs or the lungs (DVT/PE): To prevent blood clots from forming you will be given special stockings, an injection to thin the blood. During and immediately after your operation you will also wear special boots to prevent clots from occurring. You need to continue to wear the stockings for few weeks after your operation.
- Smoking significantly increases the risk of clotting. If you are a smoker, you will be advised to stop smoking before surgery.
- Vomiting/Band intolerance: very occasionally the stomach may respond to surgery and the insertion of the band with frequent spasms and a temporary intolerance to food and even liquids. This is a rare and unpredictable event which usually does not last longer than few days. Exceptionally may require the band to be removed.
LONG TERM COMPLICATIONS AFTER GASTRIC BAND SURGERY
- Specific to this operation, there is a 10-20% risk of complications within the first 5 years. These can include the band slipping or moving into the stomach, an increase in the size of the stomach or gullet (esophagus), rupture of the ring. This may result in the band or port needing to be removed, repositioned or replaced. One in 5-10 patients will need further surgery within 5 years.
- narrowing (structure) of the joining between the new stomach and the bowel which can make eating and drinking more difficult. This will usually settle on its own although sometimes it will need to be stretched with an endoscopy
- Hair loss or thinning in the first six months. This is a temporary side effect of the rapid weight loss and it will re-grow
- Gallstones
HOW SHOULD YOU PREPARE FOR THE PROCEDURE?
- Prepare a list of written questions for your surgeon
- Read information on websites and Weight Loss info.
- Discuss the operation with your close friends and family.
- Meet other patients
- Make healthier changes to your lifestyle
- Two weeks before the operation you will be required to follow a low calorie liquid diet. This will help shrink the liver and make the operation easier for the surgeon and safer for you.
THE DAY OF THE OPERATION
You will usually be admitted to the hospital on the day of your operation. You must not have anything to eat or drink (this includes chewing gum and calorie free mints) from 8 hours before your surgery, although you may drink plain water up until 2 hours before. In doubt please ask the surgeon or the duty nurse.
Once your admission is complete you will see your surgeon and the anesthetist and a written informed consent will be signed. You will then go to the theatre where the anesthetist put you to sleep. You will also be given an intravenous drip so you can have fluids during the operation.
WHAT SHOULD YOU EXPECT AFTER THE PROCEDURE?
THE FIRST FEW HOURS AFTER THE OPERATION
You will wake up in a recovery room where nursing staff will monitor you for any complications. You will have a drip and may have a urinary catheter and a drain into the wound. You will also be wearing stockings and have a pumping device on your legs to prevent blood clots. As soon as you are fully awake and comfortable, you will be transferred to either the surgical ward or the intensive care unit where your relatives can visit you. You will receive painkillers to control any pain. Your surgeon will instruct you when you may start to drink water, it is important you do not have anything to drink until your surgeon feels it is appropriate for you to do so.
You will be encouraged to get out of bed as soon as possible after surgery. This helps to reduce the chance of post operative complications such as blood clots in the legs or chest infections.
THE DAY AFTER THE OPERATION
The amount you may drink will be increased every couple of hours until you are able to take at least one glass of water every hour. Your drip will be removed when you are drinking enough to keep you hydrated.
You should start to feel better very quickly after the operation and will be able to move around on your own.
You need to drink one 125ml glass of smooth fluid every hour when you are awake. For example you may have tea and coffee, milky drinks and soup with no lumps. The days after surgery you will be able to go home.
AT DISCHARGE
PAIN AND MEDICATION
Gastric band is usually not a painful procedure. You will be given a supply of soluble painkillers to take home with you; these should be taken regularly for the first few days. If you have no pain gradually reduce the number of tablets you are taking. Allow soluble tablets to stop fizzing before you drink them. You will also prescribed an anti-acid tablet to be taken daily for at least three months after your surgery.
If you have been taking medication to control your blood pressure or diabetes, these will be reviewed before your discharge. Please make sure you are clear about this before you leave the hospital.
Please note: Do not take any large tablets for first two weeks as they may get stuck All tablets have to be crushed or taken in soluble form. If in doubt please ask your surgeon
Wounds
The small incisions made for your surgery will be more or less healed by the time you leave hospital. You will only need to go home with dressings. If any concerns, please remember that you can always refer to your surgeon.
ANTI-EMBOLI STOCKINGS
You should take them home with you and continue to wear them until you are walking about on a regular basis. If you are flying within six weeks from surgery, you should wear them during the flight.
EATING AND DRINKING
You will be given a diet information sheet. You should have this with you at all times so you know what to drink and are familiar with the stages of food introduction in the next few weeks. In case of doubt you are advised to contact your dietician.
WASHING
You can have a shower but do not soak in the bath for at least a week after surgery.
DRIVING
You may drive as soon as you can comfortably wear a seat belt and are able to perform an emergency stop (independently assessed by a close relative or a friend). You should check with your insurance company for their specific advice about driving after keyhole (laparoscopic) surgery.
OTHER ACTIVITIES
You will be able to walk straight after surgery. Try to go for a walk every day, gradually increasing the distance as you feel able. You will probably need at least 2 weeks off work but please check with your surgeon. It is advisable to avoid heavy lifting for at least 1 month after abdominal surgery, if you are unsure discuss with your surgeon. You may resume sexual activity as soon as you feel comfortable.
Women of childbearing age must not become pregnant for at least one year following gastric band surgery. After one year: if you are planning a pregnancy please contact your dieticians for nutritional advice.